An Abbotsford senior is now recovering from third-degree burns, infection and skin-graft surgery at Vancouver General Hospital, after local doctors repeatedly concluded that her burns weren’t serious.
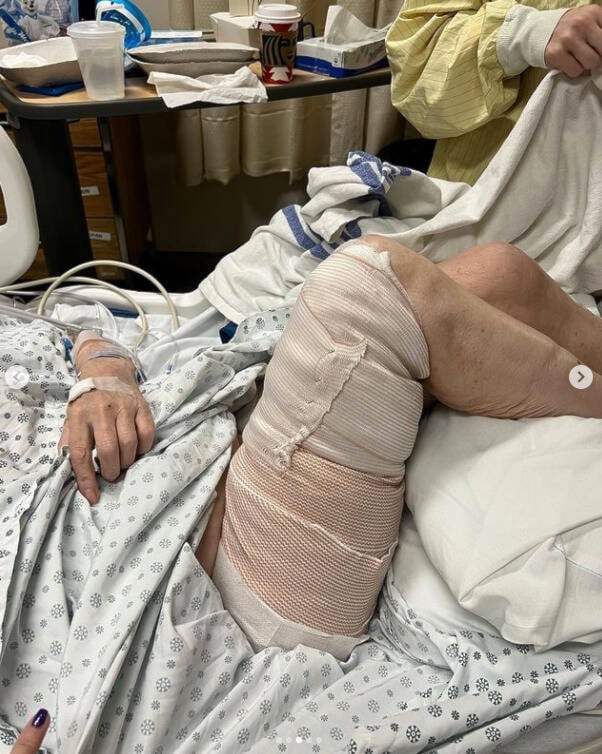
On Dec. 12, 75-year-old Ruth Harris was making some soup when she accidentally spilled the entire contents of a boiling kettle into her lap. The result was third-degree burns on the insides of her thighs, says her daughter, Maureen Keyes.
But this diagnosis came a grueling three weeks after the incident, when the burn team at VGH saw photographs of Harris’s legs. By then, the burns had become badly infected.
The delay in surgery wasn’t for lack of trying to get medical help, Keyes told The News. She has been Harris’s full-time caregiver for 12 years, following a stroke that left her mom partially paralyzed and non-vocal. They live together, along with Keyes’ husband and their daughter.
“I’m her voice,” she said.
When the accident happened, she called an ambulance immediately and got her mom to the emergency department at Abbotsford Regional Hospital. The staff there tried to release Harris back to Keyes’ care at 1 a.m., giving them some wound dressing supplies and saying they were just first- and second-degree burns.
“They said, ‘You have to take her,’ ” Keyes recalls, but she talked them into keeping her there. The next day they called again, and Harris was sent home.
Over the course of four days the burns got worse and worse at home, and Keyes took her mom back to the ER on the advice of a friend who is a nurse. Eventually, Harris was admitted to a medical ward, but Keyes says that was likely due to her suffering caregiver burnout and having a breakdown.
On Christmas Day, hospital staff wanted Harris to go home again, as she was done her antibiotics. But her needs had increased so much over the weeks that Keyes did not feel equipped to care for her there.
She learned about the burn unit at VGH and started demanding that her mother be seen there.
“I myself had to get the burn clinic’s number,” Keyes said. “I organized the appointment directly. I had to arrange the hospital transfer because they (the new patient care coordinator) didn’t know how to do it.”
At some point, ARH staff agreed to send Harris to VGH to be seen at the burn unit. One hospital transfer process was wrought with confusion, sending Harris to St. Paul’s by mistake. Luckily, St. Paul’s staff took a look at her burns and sent photos to VGH. They determined Harris had “intensive medical needs.”
VGH doctors booked her in immediately for the skin graft surgery.
“She needed this surgery three weeks ago,” the doctor told Keyes over the phone that night. “Be ready for surgery in the morning.”
What Keyes didn’t know before that is that third-degree burns don’t heal on their own. Harris has now had skin graft surgery from the sides of her legs and can begin the healing process.
Now that her mom is on her way to healing, Keyes is examining all the things that went wrong in Abbotsford. One of the main problems she says was timing, and that could not be helped. Their family doctor was away for holidays and wasn’t aware one of her patients was in the hospital with burns.
That left Keyes as the sole advocate for her mom.
Harris and Keyes used to run their dance studio together, Xtreme Talent Dance Company.
Keyes describes her mom as well-loved and independent. For example, she is still able to use the washroom on her own and able to communicate in many ways despite not speaking. She is cognizant, aware and often the life of the party. She even stays home alone with the family’s pets for a day or two at a time, caring for them and herself.
Keyes says that’s why it was hard to watch her deteriorate, both at home and once she was admitted properly. When she was eventually admitted to a general ward, Harris was placed in a second bed in a single-bed room. Due to the tight space, her wheelchair was removed and she was given a pad to pee on instead.
At one point, a doctor called and referred to Harris as a dementia patient and brought up end-of-life care. Keyes said that while communicating with someone who has had a stroke can be difficult, it’s not the same as dementia.
Complicating everything were staffing issues at the hospital over Christmas. The patient care coordinator in charge of the file was brand new to the job, Keyes said, which caused part of the confusion around hospital transfers.
But the continued insistence from a doctor there that the injuries weren’t third-degree burns is the most concerning, she said.
“I have so many stories I could tell,” Keyes said, including her mom not being given an intravenous drip, nobody mentioning infection, and being given the wrong supplies for the wound care when they were initially sent home.
Now, she’s worried about her mother’s care when she’s eventually released from Coastal Health and “repatriated” back to Fraser Health.
Harris makes just a bit too much to eligible for home-care coverage. Keyes still runs the dance studio, along with raising her daughter. She’s also a student at University of the Fraser Valley. But since she had to miss the whole first week of classes this semester, she made the difficult choice to take a semester off.
“She’s been a lot of work for me but I love her to death,” Keyes says. “The staff at Coastal Health have moved mountains for us.”
And while she’d been dealing with caregiver burnout, and missing a semester of school, she said she’s happy to devote her time and energy to her mom.
“I will give everything and anything to give her life meaning,” she said. “She doesn’t have a lot of time left, and I refuse to have her waste away. She deserves to live a life, and is loved by a lot of people.”
When Keyes tried to file a complaint with Fraser Health, the links they provide to the ombudsman were broken, she said. She will be filing complaints as necessary, she adds, and exploring different ways to find the right care for her mom when she comes home to recover. She is also chronicling the ordeal on her Instagram page.
“I’m disappointed,” Keyes said.
Fraser Health provided the following response to a series of questions posed by The News, through a communications officer.
“We are sorry to hear that the family of a patient who received care at Abbotsford Regional Hospital has concerns about the care their loved one received while in our hospital. We have connected with the patient’s family directly to hear their concerns, including ensuring the patient has a care plan in place when they return home.
“Each patient’s care journey is unique, depending on their circumstances and clinical needs, and particularly if they require treatment for burns.
“When patients are admitted to Abbotsford Regional Hospital, under a medical program, they are supported by a hospitalist who is part of a team specializing in general hospital-based medical care. The hospitalist is responsible for the patient’s care plan and coordination including all referrals, diagnostics and treatment. When a patient has a family physician, physician reports, results and patient summaries are copied to the family physician to ensure they are informed and able to appropriately support their patient following discharge.
“We have processes in place to ensure that all patients who require additional care in other facilities or regions are directed to the appropriate facility in which they are booked by their physician.
“Upon discharge from hospital, community-based home health and home support services are available to support patients who need additional support when they return home. If a patient requires home health or home support, Fraser Health follows the appropriate Ministry of Health processes. Rates and charges follow the policy according to income, though there are mechanisms to apply for hardship under certain conditions.
“In general, when patient volumes are high in our hospitals, we may use alternative spaces to provide support to our patients. These spaces align with all infection prevention and control guidelines and patients receive the care and supports they need. Patients who need a higher level of care are supported in private or semi-private rooms.
“We are committed to supporting all patients in maintaining their baseline level of activity and capability, including toileting. Depending on where a patient is being provided care, toileting may be more challenging in some locations and alternatives such as commodes may be used on occasion.”
@CHWKcommunity
jessica.peters@abbynews.com
Like us on Facebook and follow us on Twitter.