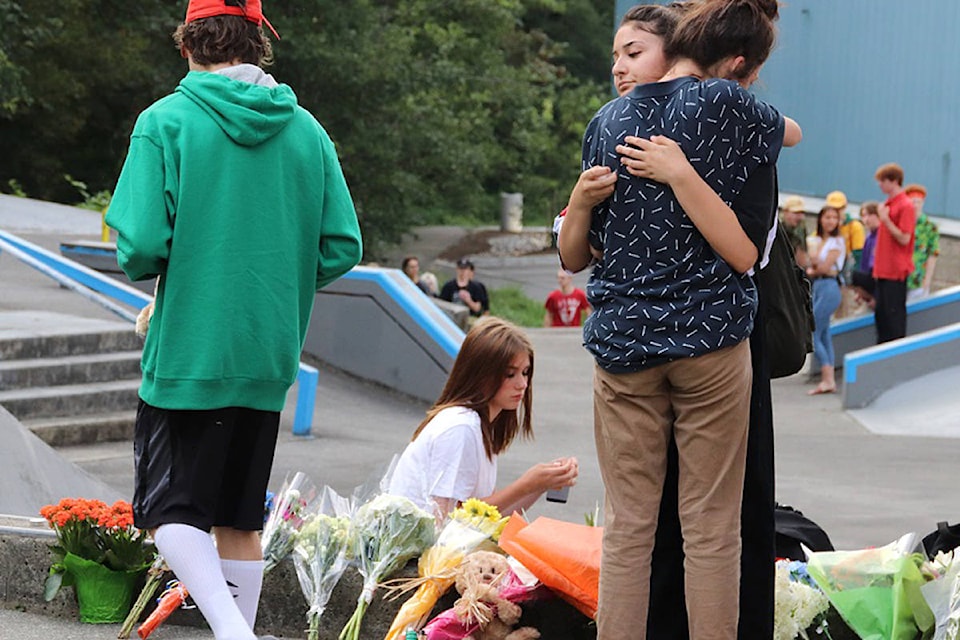The overdose crisis in B.C. has reached all corners of the province, impacting all ages, regions and income-levels.
Most vulnerable are the children and youth whose lives are taken too soon, affecting friends and classmates, and sparking difficult conversations for parents.
Last week, 14-year-old Carson Crimeni tragically died in an apparent overdose at a Langley skateboard park. Distressing videos of him circulated on the social media platform Snapchat just hours before he was found unresponsive near the park. He died a short time later in hospital.
It’s believed none of the youths filming or seen in the videos called 911 when Crimeni went into critical condition.
The secondary school where he was soon to be entering Grade 10 released a statement, urging parents and guardians to speak with their kids about the incident, while grief counsellors were made available.
Shortly after, 16-year-old Abby Barker died of a suspected overdose in an unrelated incident in Greater Victoria.
WATCH: Evening vigil draws hundreds after death at Langley skate park
But talking to children about drugs can prove complicated. Parents must combat misinformation and pro-drug messaging on social media while educating themselves on evidence-based harm-reduction strategies such as naloxone kits and the legal system.
Dr. Carol Ann Saari, a child and adolescent psychiatrist at BC Children’s Hospital, told Black Press Media that parent-child drug talk should begin once the child starts showing curiosity. That said, parents shouldn’t feel the pressure of explaining everything there is to know in one discussion.
“This isn’t a single conversation, this is a series of conversations and communication that go on for many years, and the conversations need to start quite young – so starting when the kids are in elementary school or at least by middle school” Saari said in a phone interview.
Those conversations may start with what drugs are, what they can do and their risks, she added.
The B.C. government declared the staggering rise in overdose deaths a public health emergency in mid-2016. More than 2,400 people have fatally overdosed across the province since then, with 80 per cent of those linked to street-level fentanyl. In most cases, the illicit narcotics are unknowingly mixed into other drugs, such as crystal meth, cocaine and heroin.
Twenty-four teens under the age of 18 fatally overdosed in 2017, and a further 18 died last year.
Drug hysteria has been a fixation of North American policy for decades, including the zero-tolerance “Just Say No” campaign started by Nancy Reagan in the 1980s and the DARE program which has since been intertwined in pop-culture references.
But fear-provoking “drugs are bad” lectures can sometimes backfire, Saari said.
READ MORE: West Shore students mourn the loss of another classmate
“Kids start to not believe some of the stories they are hearing because they also see a lot of stuff on social media, they see a lot of movies, where people are using substances and they are not having these horrible outcomes,” she said. “There has to be a bit of a balanced view that’s brought to kids.”
Some parents fear acknowledging the elephant in the room too soon could be perceived as encouraging drug and alcohol use. But Saari said not talking about it leaves a gap for misinformation to fill.
“If you don’t talk about it and kids have curiosity, then they are going to talk to somebody,” she said. “And if they can’t get guidance from their parents, with a balanced view and who have their best interests then they are going to go to their peers, who also have their limited information, as well, and so it is the blind leading the blind”
Conversations can include the risks of drugs – especially the Russian-roulette-like turmoil fentanyl has created within street-level opioids and narcotics. Discussions can also include what to do if a teen feels worried about their own drug use, or about their friends, and how to respond to peer pressure.
In May 2017, the federal government enacted the Good Samaritan Drug Overdose Act, which gives criminal amnesty from drug possession for anyone who calls 911 to report an overdose. In other words: If a Canadian is around drugs or impaired on drugs, they will not be arrested for calling emergency officials because someone is overdosing or suspected of overdosing.
Meanwhile, naloxone is available for free at most pharmacies across the province. Community groups, school districts and organizations such as Toward The Heart often host training sessions for what to do in the case of an overdose, including how to administer naloxone.
Take Home #Naloxone kits now available at community pharmacies in BC. Learn how to save lives at https://t.co/aDqfdLSuvu. Find a site to get a kit at: https://t.co/XI63Bzpg5H pic.twitter.com/eKXSEfN7Hh
— Toward the Heart (@towardtheheart) December 21, 2017
Saari said having a dialogue that encourages safety and openness instead of placing blame on those suffering from addiction can create a place of trust as children find themselves facing new situations.
That can include planning together how a child can ask for help if stuck in an uncomfortable situation. Saari said she’s seen parents and kids have a code word they can send through text that prompts a phone call from mom or dad saying that it’s time to come home.
READ MORE: Fundraiser launched for family of teen found dead at skateboard park
“We know that we are not going to be able to stop kids from experimenting, I think that it’s built into our DNA that people try things,” she said.
“We want to try and delay that as much as we can, and keep them alive and keep them safe… to allow for them to come to you and not feel like they’re going to be punished if they are opening up to you.”
For information on how to talk to your child about substance use, and other resources, click here.
@ashwadhwani
ashley.wadhwani@bpdigital.ca
Like us on Facebook and follow us on Twitter.